Have you ever found yourself standing in the shower and hand expressing just a drop of milk to see if there’s any? Yeah, it happens, and I can assure you, you’re definitely not alone. Breastfeeding is amazing, yet it can be overwhelming and come with so many worries and anxieties. One of these worries could be wondering if you have enough milk to feed your baby. I’m here to tell you, that true low milk supply is rare, and in most cases Mother Nature has it under control – a women’s body is designed to produce enough breastmilk to feed their babies, and when it doesn’t, there are many ways we can increase breastmilk production.
What Does ‘Normal’ Look Like?
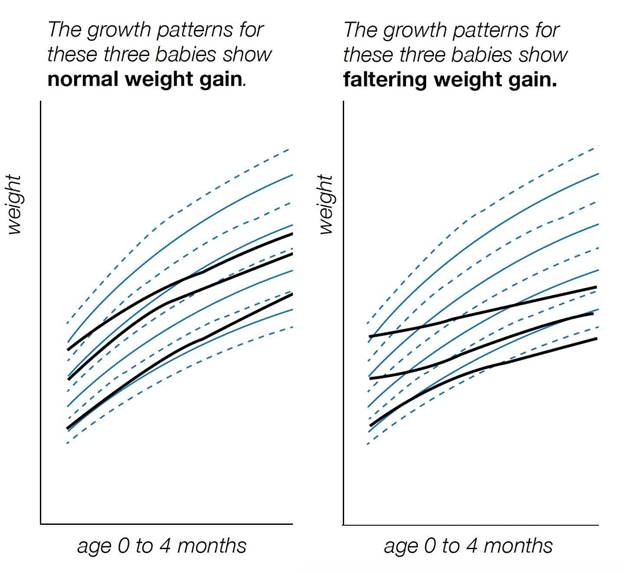
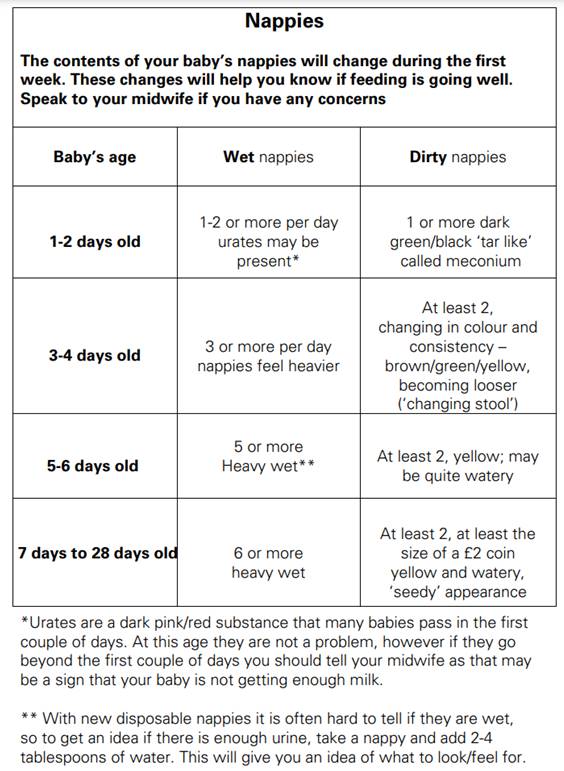
Here are some indicators, which show that everything is okay and that baby is actually getting enough milk. Let’s start with the numbers! A great sign is if baby is gaining weight properly and has made enough wet and dirty nappies throughout the day (see chart). If a baby has 8+ feedings in 24 hrs it can sometimes be difficult to tell, it can all feel like one big cluster feeding (totally normal); I’ve been there, cuddled up on the sofa hoping my phone doesn’t die on me, or that I can reach my water bottle without waking my baby after a feed. You hear many things, but in general, if the baby’s feeding lasts from 5 to 40 minutes at each feed, that is completely normal, and after day 3 or 4 when the milk comes in to replace colostrum, you should be able to hear your baby swallow.
So after looking at these numbers, let’s see how your baby is doing! You want to see your baby calm and relaxed during feeds, and content after (in general – remember the witching hour, which is heart wrenching but completely normal, you’re not alone!), baby comes off the breast on their own after feeds, their mouth looking moist, and the nipple looks more of less the same after each feed (not pinched, flattened, white, etc.). And of course the baby has a normal skin colour – not e.g. yellow (jaundice).
What Is ‘Perceived Low Milk Supply’?
Perceived low milk supply is when you believe you’re not producing enough milk – where in fact, your production is perfectly normal sufficient for breastfed babies. It’s important to remember that babies not only breastfeed for nourishment but also to seek comfort, to feel safe and secure, and it helps them to regulate their body temperature by keeping them warm, so don’t be alarmed if your baby wants to feed frequently.
Remember, a baby’s stomach is small and breastmilk can be easily digested in about 1.5-2 hours. After 2-3 months your baby should be feeding for shorter amounts of time than before (with practice, babies get more efficient at extracting the milk from the breast over time), but your baby may still want to feed for a long time (don’t forget about cluster feedings – I know, how could you, right?). It’s completely normal that your breasts feel soft, even before feeds, and that’s because between 3-12 weeks your milk supply adjusts to your baby’s needs, and as long as your baby’s feeding well you will produce enough milk for them.
Finally, if you’re not gaining much milk while pumping, don’t be alarmed! Babies are much more efficient than pumps and a mum can have great amounts of milk supply to feed their baby (even over supply) yet unable to efficiently pump.
Issues That Can Lead To True Low Milk Supply
Here are some common issues that can affect a mums milk supply, and that without resolving them, could lead to true low milk supply.
- Difficulty Latching – if a baby is not latching well to the breast, they are not extracting milk properly, over time signalling to mum’s body that less milk is needed. This could be caused by poor positioning, or due to your baby having a tongue-tie or lip-tie.
- Cutting feeds short – It’s important that both you and your baby are comfortable and that baby can finish feeds on their own without cutting them short. By cutting feedings short or supplementing with formula, rather than feeding baby responsively to baby’s cues, it could signal to your body to create a drop in milk supply.
- Mental Health & Medications – Stress, anxiety, depression, and some medications such as oral contraceptives, even some herbal/over the counter medications can all negatively impact your production. There are websites available to check if certain medications are safe to take during breastfeeding, and always make sure to consult your doctor and lactation consultant.
- Alcohol and Smoking – drinking alcohol and smoking can also have a negative impact on your milk supply.
- Fewer Milk Ducts – Some mums have fewer than normal milk ducts due to e.g. cancer or breast surgery which in turn lowers the flow of milk to baby.
- Illness – Poor health or illness in mother or baby. It’s important to note that only 5% of mothers do not experience reduced milk production due to medical reasons.
- Separation – Having to spend time away from baby after birth (e.g. premature birth) limits the natural queues your body looks for to trigger milk production.
- Obstruction – even seemingly harmless things like nipple shields can lead to reduced milk supply. Although with damaged nipples, their use might be the only way of carrying on for the time being, which is preferable to having to stop breastfeeding altogether. It’s worth noting that if there’s a need for a nipple shield, there is always an underlying issue which can be addressed and resolved by the help of the right professionals (lactation consultants, in this case).
- Irregular Feedings – As much as you might hear “Don’t wake a sleeping baby!”, it’s very important that they be woken up for feedings during the first 6 weeks. This is a vital time where your milk production is being established. Starting a feeding routine early is a good way to ensure a healthy milk supply. Sometimes babies don’t want to wake up for feedings because they don’t have the energy to wake themselves, so it’s important to wake them if necessary, every 2-3 hours during the day and at least every 4 hours during the night. If your baby keeps falling asleep during feeds, it can be helpful to take a layer of their clothing off or even feed them in their nappy. Having them on you, skin-to-skin, tickling their feet, stroking their cheek, changing sides/breasts you feed from, or changing their nappy before feeding times can help them stay awake and finish their feed – whatever works for you and your baby.
- Painful Feedings – Breastfeeding should always be comfortable for mum (and baby) – breastfeeding should never be painful for the mother. Slight discomfort in the nipple is normal in the first few days of breastfeeding, for max 5 seconds after baby latches on to the breast. If you experience discomfort for longer than that or pain while breastfeeding, seek support from a trained breastfeeding personnel as pain is an indicator of a breastfeeding problem (e.g. incorrect latch and/or position, thrush, tongue/lip-tie, etc.), which should be resolved as soon as possible, so you don’t live with pain and so it doesn’t affect your breastmilk supply.
All that said, most of the time these issues can be resolved with the right professional’s support (e.g. lactation consultant) – we all need a little help sometimes, or a lot more than that!
How To Increase Your Milk Supply?
So the big question: How to increase milk supply? First of all, for a good milk supply the mum should get as much rest as possible and lower the levels of stress – as it can affect the let-down reflex, which releases milk into your milk ducts. Obviously it’s not always easy, but it could be helpful to ask your partner, family and friends to help with other things so you can be more focused on breastfeeding and less worried over other things, especially in the first few weeks. I quite like the idea of a “nursing vacation”, where you take your baby to bed with you for 2-3 days, and do nothing but nurse as frequently as possible and rest. Even if you have older children, they could camp with you, according to your preference and options.
In general, it can be extremely useful, to have lots of skin-to-skin contact with your baby, offering both of the breasts as often as possible, switching in between the breasts in one feed, and starting feeds alternating between the sides/breasts. Ideally, do not supplement with formula, as that will reduce the milk supply, also could be helpful to pump after/in between feeds, to build up your milk supply.
Listen To Your gut
In any case, listen to your gut feeling. You know your baby best, and if you’re ever in doubt or think you might have a true low milk supply, don’t hesitate to seek help. You do not need to wait until it gets “really difficult or bad”, push aside the idea of “it’s not that bad” and reach out for help, if not just to put your mind at ease.
Message has an amazing team of Breastfeeding Supporters who can help you with all your breastfeeding questions and can signpost you to certified IBCLC lactation consultants if needed. This contact list is absolutely free for Message members and can be found at the end of all Message Magazines, online, or in the app. You’re doing an amazing job Mumma! You’ve got this!
Bibliography
- https://www.nhs.uk/conditions/baby/breastfeeding-and-bottle-feeding/breastfeeding-problems/enough-milk/
- https://www.thewomens.org.au/health-information/breastfeeding/breastfeeding-problems/low-milk-supply
- https://americanpregnancy.org/healthy-pregnancy/breastfeeding/low-milk-supply/
- https://www.laleche.org.uk/how-milk-production-works/
- https://www.laleche.org.uk/my-baby-needs-more-milk/
- How can I tell that breastfeeding is going well?
- https://kellymom.com/hot-topics/low-supply/
- https://www.allnaturalmothering.com/mom/true-signs-low-milk-supply/